CBD Facts: What a Cannabis Medicine Doc Wants You to Know
By Dr. Rachel Knox
The use of CBD in personal care products has rapidly increased over the past few years. CBD has been touted as the major “non-psychoactive” chemical in cannabis (which is a problematic distinction, and I’ll expand on that in a minute) and championed as a non-pharmaceutical gateway drug to better health.
It’s in nearly everything, too. CBD can be found in creams, patches, tinctures, capsules, chocolates, beverages, vape pens, inhalers and more; you can even find it infused into activewear. But, is the key to feeling better really as simple as “just add CBD”?
It is pretty clear that most people are buying CBD personal care products for medicinal (i.e., therapeutic) reasons, seeking relief from symptoms like chronic stress or chronic pain. This doesn’t come as a surprise when we break down American ailments.

Let’s take a quick look at the numbers: 1 in 1.5 American adults is living with chronic stress, 1 in 2 is suffering from chronic headaches, 1 in 3 is suffering from insomnia and/or prediabetes, and 1 in 5 is battling mental illness and/or chronic pain. Western medicine has not addressed these problems well enough, leaving many people looking for alternative solutions such as CBD. Consumer demand for Cannabidiol continues to rise despite ongoing confusion around the regulation of hemp cultivation and CBD production; without comprehensive education around what CBD really is, what it can do, and how it does it.
Let’s review some better and lesser known facts about CBD, and discuss what really makes a CBD product a contender.
What is CBD?
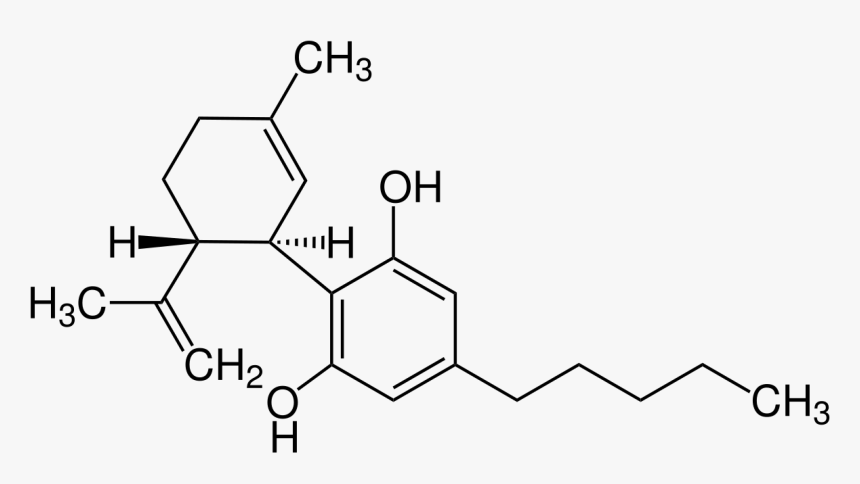
CBD is short for Cannabidiol, one of the major phytocannabinoids made by the plant genus Cannabis sativa. For those who like to really nerd out, it’s a 21-carbon molecule with a central 6-carbon ring and side chains, and was the first cannabinoid isolated and deciphered in 1963 by Israeli researcher, Dr. Raphael Mechoulam.
CBD is Psychoactive
Unlike THC, which is responsible for causing the “high” associated with cannabis, CBD is non-intoxicating. This doesn’t make it non-psychoactive. Described in literature as having anti-stress, anti-anxiety, calming, relaxing, antipsychotic, and anti-seizure properties, CBD is the textbook definition of a psychoactive drug, i.e., a substance that affects mood, motor activity, behavior, and cognition. Because CBD can affect all these things, calling it “non-psychoactive” is not a benign misnomer; it is false, unscientific, and misleading. In fact, all phytocannabinoids are psychoactive, just in different ways, and to different degrees.
This little nugget of truth isn’t meant to disappoint nor discourage. Not only is it imperative that consumers understand how CBD might affect them, it’s important that we end the pejorative association between psychoactivity and harm.
How CBD Works
Many people believe CBD works on the endocannabinoid system (ECS) through the cannabinoid receptors, but this isn’t exactly true. While THC locks directly into cannabinoid receptors (like CB1 and CB2) to cause an effect, CBD works more indirectly. One way it does this is through binding “off-site” to the CB1 receptor. This doesn’t cause a direct effect, but changes how CB1 responds to molecules that do lock directly into it, such as THC or endocannabinoids (endogenous cannabinoids aka cannabinoids made by the body).
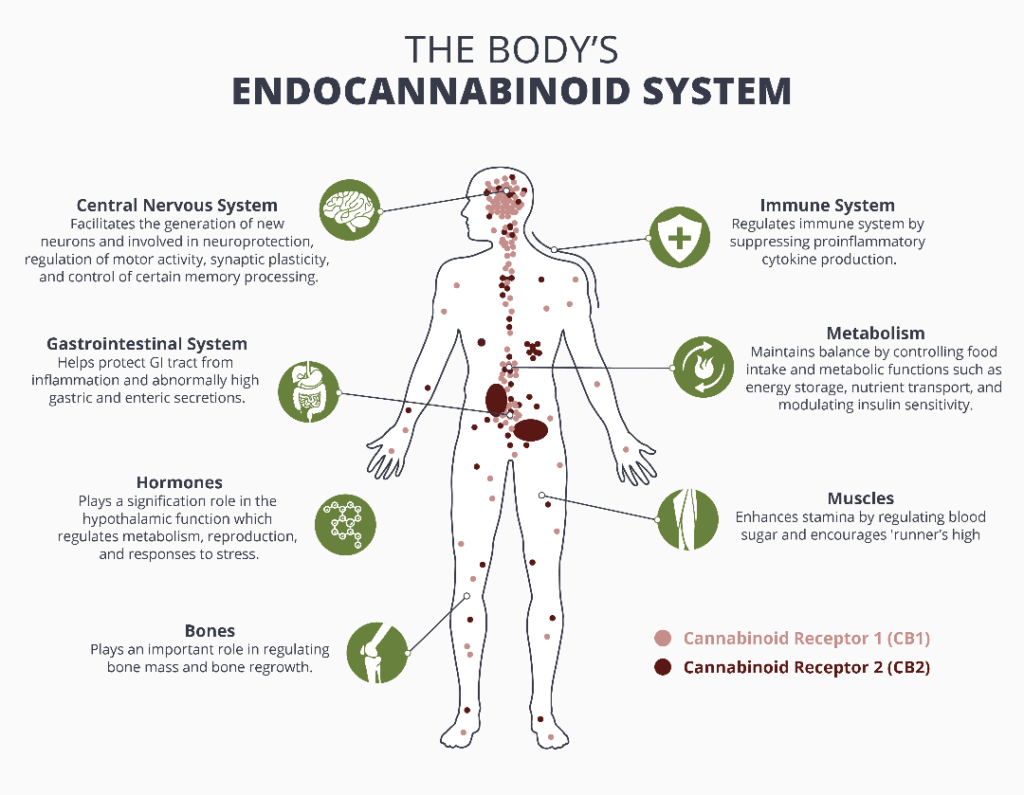
CBD also blocks the enzyme FAAH that breaks down the endogenous cannabinoids anandamide and 2-AG. This inhibition results in higher levels of endocannabinoids available to CB1 and CB2, which is important because those endogenous cannabinoids play a big role in things like feelings of well-being, sleep, inflammation and overall endocannabinoid system balance and tone.
Lastly, CBD works on over 65 other cellular receptors in the body, including pathways involving other neurotransmitters. These non-ECS targets include serotonergic, glutamatergic, opioid, and vallinoid pathways, which are highly involved in the regulation of mood, motivation, anxiety and pain.
CBD even affects the signaling molecules important in our immune system, like cytokines. Many clinician researchers believe its CBD’s indiscriminate behavior that results in such broad-ranging effects.
What are CBD’s benefits?
Many illnesses can be traced back to dysfunction in the endocannabinoid system (ECS), which is essentially designed to keep our bodies in homeostasis or balance.
Think of the ECS as the control board of health. When the control board malfunctions, the result manifests as symptoms of illness or disease. Research has shed some light on this, classifying conditions like migraine headaches, fibromyalgia, IBS, and PTSD as true endocannabinoid deficiency syndromes. Uncontrolled inflammation, chronic pain, chronic stress, seizure disorders, and cancer are also linked to ECS dysfunction.
So, how does CBD fit in?
Endocannabinoid deficiency disorders, like those listed above, are disorders involving low endocannabinoid levels. In western medicine, we treat disorders of deficiency with supplementation – think: vitamin D supplements to treat vitamin D deficiency. So when it comes to supplementing endocannabinoid deficiencies, clinician-researchers get a little creative.

Remember: CBD blocks the breakdown of endocannabinoids. Because of this, CBD may have a role in addressing endocannabinoid deficiency syndromes simply by indirectly increasing endocannabinoid levels. Clinical evidence otherwise remains limited, but ongoing research is underway, including studies on anxiety, autism, diabetes, multiple sclerosis, and Parkinson’s disease.
The only CBD preparation that has been FDA approved for the treatment of any condition is Epidiolex®. It was approved in 2018 for two treatment-resistant seizure disorders, Dravet Syndrome and Lennox Gastaut Syndrome. Research hasn’t sorted out how CBD treats seizures exactly, but it’s beyond clear that it does.
Another fact to note is that the federal government has a patent on cannabinoids as antioxidants and neuroprotectants. The 2003 patent states that cannabinoids are “useful in the treatment and prophylaxis of a wide variety of oxidation associated diseases, such as ischemic, age-related, inflammatory and autoimmune diseases,” and that “cannabinoids are found to have particular application…in limiting neurological damage following ischemic insults, such as stroke and trauma, or in the treatment of neurodegenerative diseases, such as Alzheimer’s disease, Parkinson’s disease, and HIV dementia.” Read into this what you will, but it sounds like an admission of benefit to me.
Despite the dearth of FDA-approved CBD products, consumers are still reaching for CBD to address stress, chronic pain, and inflammation at large.
Is CBD Safe?
CBD is a phytocannabinoid. It’s a single chemical and a drug. When consumers use CBD, they aren’t using just CBD. They are typically using it as a component of full- or broad-spectrum personal care products. A full- or broad-spectrum product includes other naturally occurring phytochemicals (like terpenes) extracted along with CBD, meaning that product does not contain CBD alone.
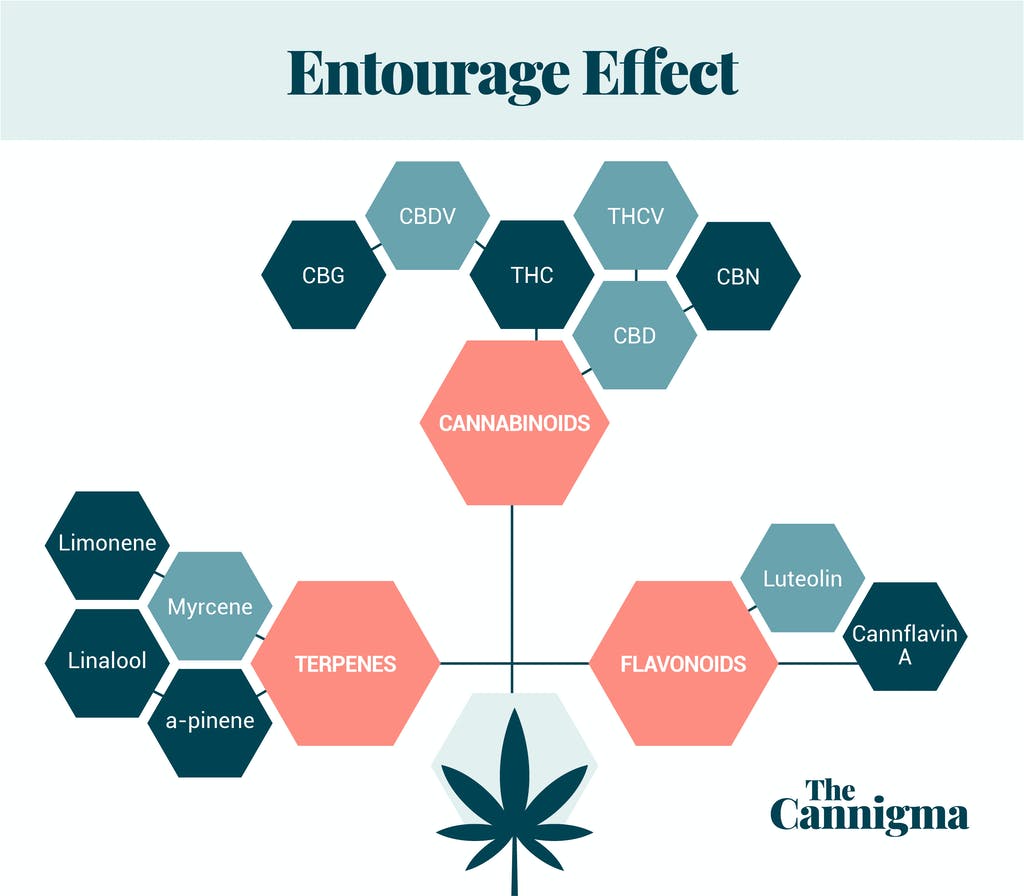
In this form, CBD is considered very safe. In clinical jargon, we use the term “risk profile” to reference the benefits of any medication in comparison to the risks (i.e., adverse effects or toxicity). Most of the adverse effects of using cannabis, such as intoxication, short-term memory loss, anxiety, and rapid heart beat can be attributed to THC and not to CBD. This is not to say that CBD personal care products are without any risks, so let’s discuss how to avoid them.
CBD Products: How to Pick a Winner
Getting the most out of a CBD personal care product begins with minimizing risk. To start, understand that cannabis is a bio-accumulator, picking up anything in the soil where it is grown, including heavy metals. It can also retain pesticide residues, or be affected by molds or mycotoxins, all of which can pose a risk to the user.
This is where Certificates of Analysis (COAs) come in handy. Be sure to evaluate the COA of the product batch your product came from to confirm that it has passed quality testing. If no COA exists, do not buy. Similarly, some CBD personal care products have been found to have higher than expected levels of THC. The COA should also report what other cannabinoids are present.
Lastly, choose CBD personal care products with purpose. Evaluate all that a given product contains, as many products are formulated with other botanical compounds and food ingredients, both natural and synthetic. Choose formulations that address your concerns, and buy from companies that align with your personal values. Not all CBD products (or companies) are created equal.
Precautions for CBD Supplementation
Remember that CBD is a pharmacologically active chemical that can have unwanted side effects, especially at high doses or when taken alone as an isolate. These side effects may include GI disturbances, fatigue, and even somnolence (aka drowsiness). One way this can be mitigated is to use full- or broad-spectrum products.
The presence of other phytochemicals significantly reduces the risk of single-chemical toxicity – even when it comes to natural substances like CBD. Another way to avoid unwanted effects is to always begin at or below the designated serving size present on every label, increasing over time until the desired outcome is reached.
Taking CBD with Other Medications
Being pharmacologically active also means there is a risk for drug interactions. Consumers taking prescription drugs should discuss CBD use with their medical doctor before use. CBD is metabolized in the liver by the Cytochrome P450 system, which is the same system that metabolizes the majority of prescription drugs. Using CBD at the same time as prescription drugs can alter their rate of metabolism, and therefore impact both their effectiveness and therapeutic window, increasing the risk of toxicity. Using CBD with prescription drugs may simply require dose adjustments, but this should be worked out under medical oversight.
Click here to view all our products!

DR. RACHEL KNOX, MD, MBA
Dr. Rachel Knox is a certified Cannabinoid Medicine specialist who received her medical and business degrees from Tufts University after completing her undergraduate studies at Duke. She trained in Family and Integrative Medicine before pursuing additional study in the areas of Functional Medicine, Cannabinoid Medicine, and Endocannabinology – the study of the function, dysfunction, and modulation of the most important physiologic system in the human body, the endocannabinoid system.
As a Cannabinoid Medicine specialist and endocannabinologist who has counseled several thousand patients in cannabis therapeutics, she has seen first-hand how significant a role cannabis and cannabimimetic modalities play in helping patients reclaim their health and overall sense of wellness, establishing renewed ownership over their lives. She has witnessed her patients safely use cannabis as adjunctive therapy to their conventional treatment plans, to wean from prescription drugs, find relief from the side effects of toxic therapies, or avoid conventional pharmaceuticals altogether.
Dr. Rachel believes that industry-wide engagement is necessary to maintain the highest standards of care and oversight, from seed to use, in the service of providing education and compassionate, wholly informed care to patients everywhere.


 The Steady Supply
The Steady Supply

 Personalized Vibes
Personalized Vibes
